In this article
AI in healthcare: practical guide for innovators in 2026
AI & Automation
Mar 24, 2026
12 min read
Discover how AI transforms healthcare operations for startups and mid-sized companies. Learn practical integration strategies, navigate ethical challenges, and implement solutions that enhance patient care and efficiency in 2026.

Healthcare AI has moved far beyond experimental labs and buzzword-filled pitch decks. Today, startups and mid-sized companies face a practical question: which AI applications actually improve patient outcomes and streamline operations without overwhelming your team or budget? Many innovators still confuse AI’s promise with its present-day capabilities, leading to misaligned investments and missed opportunities. This guide cuts through the noise to show you exactly how AI functions in real healthcare settings, what integration strategies work for different company sizes, and how to navigate the technical and ethical challenges that determine success or failure in 2026.
Key Takeaways
| Point | Details |
|---|---|
| Practical AI roles | AI in healthcare now enhances diagnostics, personalized treatment, and operational management while augmenting clinicians rather than replacing them. |
| Integration strategies by size | Startups focus on narrow AI that solves specific pain points, while mid sized companies deploy broader AI platforms that integrate multiple functions, with success depending on organizational capacity and strategic priorities. |
| Real world benefits | Real world examples show measurable improvements such as a 23% reduction in emergency department wait times, a 40% reduction in documentation time, and an 18% reduction in inventory waste. |
| Ethics and risk management | Address emerging ethical concerns and regulatory challenges early to balance innovation with patient safety and compliant deployment. |
Understanding AI’s core roles in healthcare
AI is transforming healthcare through enhanced diagnostics, personalized treatments, and intelligent operational management. At its foundation, healthcare AI encompasses machine learning algorithms that identify patterns in medical data, natural language processing systems that extract insights from clinical notes, and robotic process automation that handles repetitive administrative tasks. These technologies don’t replace clinical judgment. They augment human expertise by processing vast datasets faster than any individual could manage.
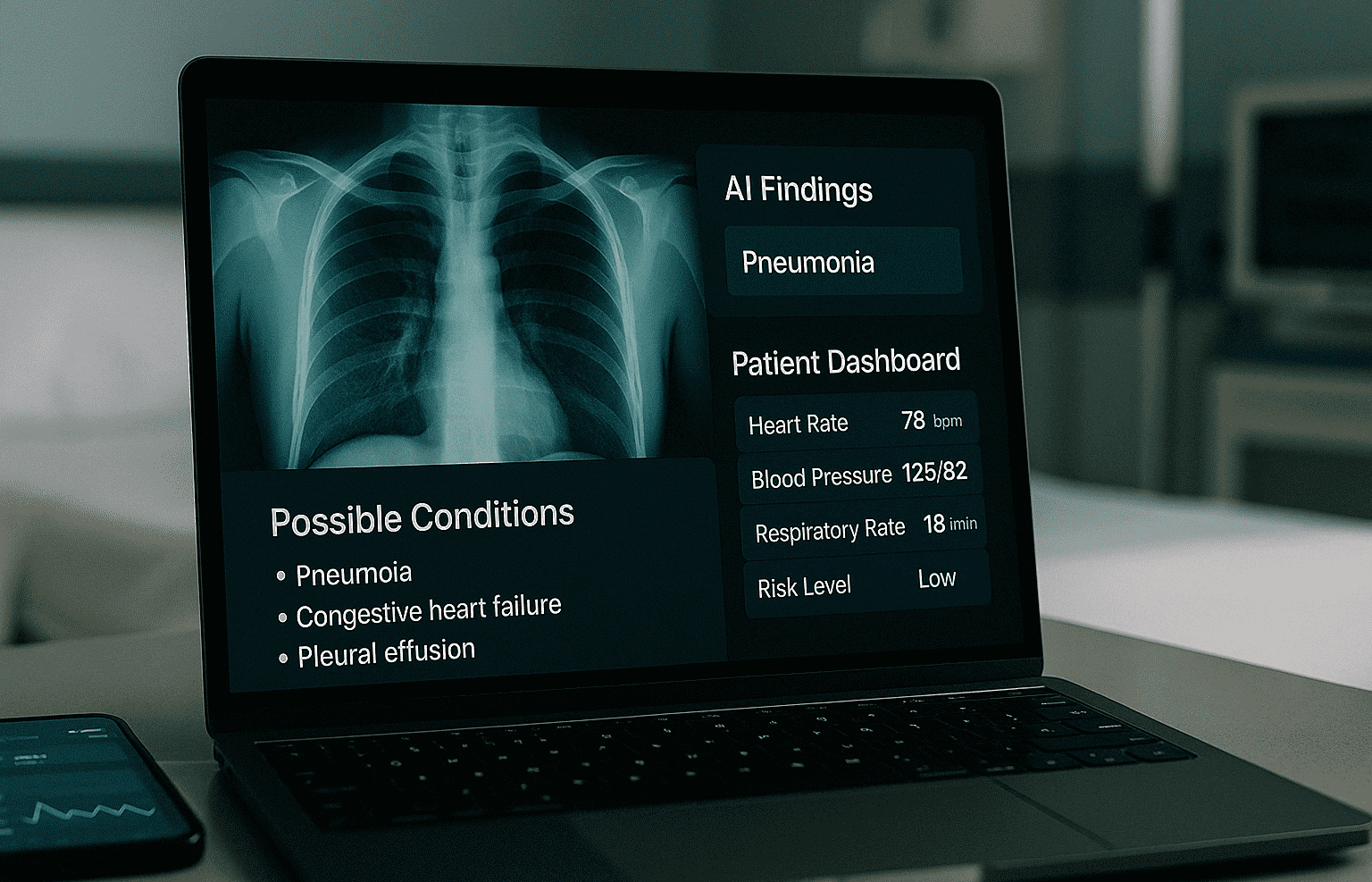
Diagnostic support represents AI’s most visible clinical application. Image recognition algorithms analyze radiology scans, pathology slides, and retinal images to flag potential abnormalities for physician review. Treatment personalization uses predictive models to recommend therapies based on patient genetics, medical history, and real-time biomarkers. Operational efficiency applications range from automated appointment scheduling to supply chain optimization and revenue cycle management.
Patient engagement tools powered by AI include:
- Chatbots that triage symptoms and answer common health questions 24/7
- Virtual health assistants that send medication reminders and track adherence
- Predictive models that identify patients at risk of missing appointments or deteriorating health
- Natural language interfaces that simplify electronic health record navigation
Startups often focus on narrow AI applications that solve specific pain points, such as automated prior authorization or clinical documentation assistance. Mid-sized healthcare companies typically deploy broader AI platforms that integrate multiple functions, from patient intake through billing. Both approaches work when matched to organizational capacity and strategic priorities. The key difference lies in implementation complexity and the infrastructure required to support ongoing AI operations.
Real-world examples demonstrate AI’s practical impact. A 200-bed hospital reduced emergency department wait times by 23% using predictive analytics to optimize staffing. A telehealth startup cut documentation time by 40% with ambient clinical intelligence that generates visit notes from natural conversation. An outpatient surgery center improved inventory management and reduced waste by 18% through demand forecasting algorithms. These aren’t theoretical benefits. They’re measurable improvements that directly affect patient experience and financial performance.
Comparing AI integration strategies in healthcare startups and mid-sized companies
Successful AI adoption requires tailored strategies based on company size and operational complexity. Startups and mid-sized healthcare organizations face different constraints, possess varying levels of technical maturity, and pursue distinct competitive advantages. Understanding these differences helps you choose implementation approaches that match your reality rather than aspirational vendor promises.
| Factor | Healthcare startups | Mid-sized companies |
|---|---|---|
| AI maturity | Early exploration, limited prior experience | Some existing systems, growing sophistication |
| Budget allocation | $50K-$250K for initial pilots | $500K-$2M for integrated solutions |
| Technical resources | 1-3 data scientists, outsourced development | 5-15 person internal teams, vendor partnerships |
| Integration complexity | Simpler tech stacks, fewer legacy systems | Multiple interconnected platforms, EHR dependencies |
| Risk tolerance | Higher appetite for experimentation | More conservative, compliance-focused |
| Primary benefits | Speed to market, competitive differentiation | Scalability, operational optimization |
Startups typically begin with cloud-based AI services that require minimal infrastructure investment. They prioritize rapid deployment and iteration, accepting some technical debt in exchange for faster market validation. Common challenges include limited training data, difficulty attracting AI talent, and uncertainty about which use cases will generate sustainable revenue. The advantage lies in organizational agility. You can pivot quickly when early assumptions prove wrong.

Mid-sized companies face integration complexity that startups avoid. Existing electronic health records, billing systems, and clinical workflows create dependencies that constrain AI architecture choices. These organizations need robust data governance, change management processes, and stakeholder alignment across multiple departments. Implementation timelines stretch longer, but successful deployments achieve broader impact across the enterprise.
Workforce readiness differs significantly between organization types:
- Startups recruit AI-native talent comfortable with uncertainty and rapid change
- Mid-sized companies must retrain existing staff while managing resistance from clinicians skeptical of algorithmic decision support
- Both face shortages of professionals who combine healthcare domain expertise with technical AI skills
Pro Tip: Start every AI initiative with a tightly scoped pilot project that delivers measurable value within 90 days. This approach builds organizational confidence, demonstrates ROI to stakeholders, and reveals integration challenges before major resource commitments. Choose pilots with clear success metrics, engaged clinical champions, and minimal dependencies on other systems.
The most successful healthcare innovators treat AI adoption as an ongoing capability-building exercise rather than a one-time technology purchase. They invest in data infrastructure, establish cross-functional AI governance committees, and create feedback loops that continuously improve model performance based on real-world outcomes.
Navigating challenges and ethical considerations in healthcare AI
Addressing privacy, bias, and regulatory compliance is essential to trustworthy AI in healthcare. Technical capabilities mean nothing if patients refuse to share data or regulators block deployment due to safety concerns. The challenges you’ll encounter fall into three categories: technical barriers, regulatory requirements, and ethical obligations that extend beyond legal minimums.
Top technical and operational challenges include:
- Data privacy and security vulnerabilities that expose protected health information
- Algorithmic bias that produces different accuracy rates across demographic groups
- Model interpretability gaps that prevent clinicians from understanding AI recommendations
- Integration friction with legacy systems not designed for AI workflows
- Validation requirements that demand extensive testing before clinical deployment
- Ongoing monitoring needs to detect performance degradation over time
Regulatory frameworks continue evolving as agencies struggle to keep pace with AI innovation. The FDA now classifies certain AI algorithms as medical devices requiring premarket approval. HIPAA compliance extends to AI systems that process protected health information, demanding encryption, access controls, and audit trails. State privacy laws add another compliance layer, with requirements varying significantly across jurisdictions. European healthcare organizations face GDPR constraints that limit data sharing even for algorithm training.
Ethical AI practices build the patient and provider trust that determines long-term adoption success. Transparency about when AI influences clinical decisions helps maintain the human-centered care that patients expect. Diverse training datasets reduce bias, but you must actively test for disparate performance across age, gender, race, and socioeconomic groups. Human oversight mechanisms ensure that algorithms augment rather than replace clinical judgment, preserving accountability when outcomes fall short.
Healthcare AI systems must maintain clear accountability chains. When an algorithm contributes to a clinical decision, both the technology provider and the healthcare organization share responsibility for validating accuracy, monitoring performance, and addressing errors that harm patients. This shared accountability model protects patients while encouraging continued innovation.
Patient consent presents particular challenges in AI contexts. Traditional informed consent processes don’t adequately explain how algorithms use personal health data or what risks algorithmic errors might create. Forward-thinking organizations develop AI-specific consent frameworks that give patients meaningful control over whether their data trains models and how AI influences their care.
The interpretability challenge deserves special attention. Black-box algorithms that provide recommendations without explanation undermine clinical autonomy and create liability exposure. Explainable AI techniques that show which input features drove specific predictions help clinicians validate algorithmic reasoning and catch errors before they affect patient care. This transparency also supports regulatory submissions by demonstrating that your AI behaves predictably and safely.
Practical steps to implement AI solutions that enhance care and efficiency
Stepwise deployment and cross-functional collaboration maximize AI benefits while mitigating risks. Moving from AI strategy to operational reality requires structured planning, disciplined execution, and continuous learning from both successes and setbacks. The implementation framework below provides a proven path that healthcare innovators have used to deploy AI solutions that actually work.
Implementation phases with realistic expectations:
- Needs assessment and use case prioritization: Identify operational pain points and clinical workflows where AI delivers measurable improvement. Engage frontline clinicians and staff to understand current process inefficiencies. Evaluate potential use cases based on data availability, expected ROI, and alignment with strategic priorities. This phase typically requires 4-6 weeks and minimal financial investment beyond internal staff time.
- Technology selection and vendor evaluation: Compare build versus buy options based on your technical capacity and timeline constraints. Assess vendor solutions for regulatory compliance, integration capabilities, and evidence of real-world performance. Request references from similar healthcare organizations and conduct proof-of-concept testing with your actual data. Budget 8-12 weeks and $25K-$75K for thorough evaluation.
- Pilot implementation and validation: Deploy AI solution in controlled environment with defined success metrics and feedback mechanisms. Train users, monitor performance daily, and document both technical issues and workflow impacts. Collect quantitative outcomes data and qualitative user feedback. Pilot phases run 12-16 weeks with costs ranging from $100K-$300K depending on solution complexity.
- Scaling and enterprise integration: Expand successful pilots across additional departments or patient populations. Integrate AI outputs with existing clinical and administrative systems. Establish ongoing monitoring processes and model retraining schedules. Scaling requires 6-12 months and $300K-$1M+ investment for mid-sized organizations.
| Phase | Timeline | Investment | Expected outcomes |
|---|---|---|---|
| Needs assessment | 4-6 weeks | $15K-$30K | Prioritized use case roadmap |
| Technology selection | 8-12 weeks | $25K-$75K | Vendor contracts, technical architecture |
| Pilot implementation | 12-16 weeks | $100K-$300K | Validated performance metrics, user feedback |
| Enterprise scaling | 6-12 months | $300K-$1M+ | Operational integration, sustained ROI |
Best practices for stakeholder engagement and data management:
- Form cross-functional AI governance committee with clinical, IT, compliance, and executive representation
- Establish data quality standards and implement validation processes before algorithm training
- Create change management plan that addresses workflow disruptions and provides adequate training
- Develop monitoring dashboards that track both technical performance and business outcomes
- Build feedback loops that capture user concerns and incorporate improvements iteratively
- Document all decisions, testing results, and performance metrics to support regulatory submissions
Pro Tip: Implement continuous monitoring systems from day one of pilot deployment. Track not just algorithm accuracy but also user adoption rates, workflow efficiency changes, and unintended consequences. Early detection of performance issues or user resistance allows rapid course correction before problems become entrenched. Set automated alerts for accuracy thresholds and review dashboards weekly during initial rollout.
Successful AI implementation requires executive sponsorship that persists through inevitable challenges. Algorithms that perform well in testing may struggle with real-world data variability. Users resistant to workflow changes may circumvent AI tools rather than embrace them. Budget overruns and timeline delays test organizational commitment. The healthcare organizations that succeed with AI treat these obstacles as expected parts of the journey rather than reasons to abandon promising initiatives.
Data infrastructure often determines AI success more than algorithm sophistication. Clean, well-structured data enables accurate predictions. Fragmented data scattered across incompatible systems dooms even the most advanced machine learning models. Invest in data integration, quality improvement, and governance frameworks before selecting specific AI applications. This foundational work pays dividends across multiple use cases rather than benefiting only a single algorithm.
Explore Meduzzen’s AI and healthcare software services
Transforming healthcare operations with AI requires both technical expertise and deep understanding of clinical workflows, regulatory requirements, and patient safety imperatives. Meduzzen’s artificial intelligence services and custom healthcare software development combine 10+ years of experience with 150+ engineers who specialize in building scalable, compliant solutions for healthcare innovators.
Our teams integrate seamlessly with your organization to develop AI-powered diagnostic tools, predictive analytics platforms, and intelligent automation systems tailored to your specific operational challenges. Whether you’re a startup validating your first AI use case or a mid-sized company scaling proven solutions across your enterprise, we provide the technical talent and healthcare domain expertise that turns AI strategy into measurable patient and business outcomes. Explore our web services and solutions to see how we help healthcare organizations build the digital infrastructure that supports advanced AI capabilities.
Frequently asked questions
What are the main benefits of AI in healthcare?
AI improves diagnostic accuracy by detecting patterns human clinicians might miss in medical images and lab results. It personalizes treatment recommendations based on individual patient characteristics and outcomes data from similar cases. Operational automation reduces administrative burden, allowing clinical staff to focus on direct patient care. Enhanced patient engagement through intelligent interfaces improves adherence and satisfaction.
How can startups effectively start integrating AI in healthcare operations?
Start with narrowly defined pilot projects focused on high-impact pain points where success metrics are clear and measurable. Engage both clinical and IT stakeholders from project inception to ensure solutions address real workflow needs. Measure results rigorously and iterate based on user feedback before committing to enterprise-wide deployment. Choose cloud-based solutions that minimize infrastructure investment while you validate product-market fit.
What ethical concerns should decision-makers watch for when deploying AI?
Ensure robust patient data privacy protections and obtain informed consent that explains how AI uses personal health information. Avoid algorithmic bias by training models on diverse datasets and testing performance across demographic groups. Maintain transparency about when AI influences clinical decisions and preserve human oversight to ensure accountability. Regular audits of AI system performance help identify and correct issues before they harm patients.
Which AI technologies are most impactful for midsize healthcare providers?
Natural Language Processing streamlines clinical documentation by automatically generating visit notes from physician-patient conversations. Predictive analytics identifies patients at high risk for hospital readmission or chronic disease progression, enabling proactive interventions. Robotic Process Automation handles repetitive administrative tasks like insurance verification and appointment scheduling. These technologies deliver measurable ROI while requiring less technical infrastructure than advanced diagnostic AI.